A vaginal / pelvic organ prolapse is when a pelvic organ slips down into the vaginal space, bulging uncomfortably (and often painfully) into the vagina. Developed prolapses can eventually protrude outside of the vagina, taking the vaginal walls with it. In each case the prolapse has occurred because the pelvic floor muscles have been weakened and can no longer do their job of holding everything in place. There are many reasons why your pelvic floor muscles can weaken. It could be as a result of pregnancy, childbirth, being overweight or obese, the menopause, heavy lifting, persist coughing, or performing regular high intensity exercise. Take a look at our causes and symptoms section for more details and what early warning signs you can look out for.
Vaginal prolapses are uncomfortable and painful, not to mention embarrassing. They can cause symptoms like urinary or faecal incontinence and can affect our enjoyment of sex. But you may be surprised to know that vaginal prolapse is a serious condition that affects far more women than you would think. In fact, around 40% of us will be affected by the time we reach our 60's! So how can we avoid being one of the 40%? There are a few simple lifestyle changes that will significantly reduce your risk of developing a vaginal prolapse while improving your overall health. These tips can even help relieve symptoms, if you have begun to experience a prolapse, and reduce the degree of your prolapse.
1. Do Your Kegels!
With a name like Kegel8, you won’t be surprised to hear that Kegel (pelvic floor) exercises are our Number One recommendation for protecting yourself against developing a vaginal prolapse. As a vaginal prolapse happens when your pelvic floor muscles become too weak to hold your organs in place, the best way to stop it is to keep your pelvic floor muscles strong via daily pelvic floor Kegel exercises. You can do these manually or make use of an electronic pelvic toner.
- Electronic pelvic toners can be used to get an even quicker and more effective improvement. They contain programmes specifically designed to the condition you are treating (or preventing).
- Biofeedback tools are also available, to help you find those all important pelvic floor muscles, and measure your improvements.
- Apps like the NHS squeezy app can be used to set out an exercise plan, monitor your progress, and remind you when your next exercise is due.
2. Breathe Deeply

We breathe in and out thousands of times a day without thinking. That's why it may surprise you to find that it's possible to breathe incorrectly, especially when it comes to maintaining a healthy pelvic floor.
When you breathe in and out deeply, the air reaches deep down into your lungs. This pushes your diaphragm and internal organs down, gently stretching and contracting your pelvic floor. By ensuring that you breathe deeply you could be making your pelvic floor stronger all day, every day!
It might sound tricky to change something that you’re not even conscious of, but it is possible if you practice for a few minutes each day. Yoga and meditation can help, as well as being a great way to relieve stress.
3. Perfect Your Posture
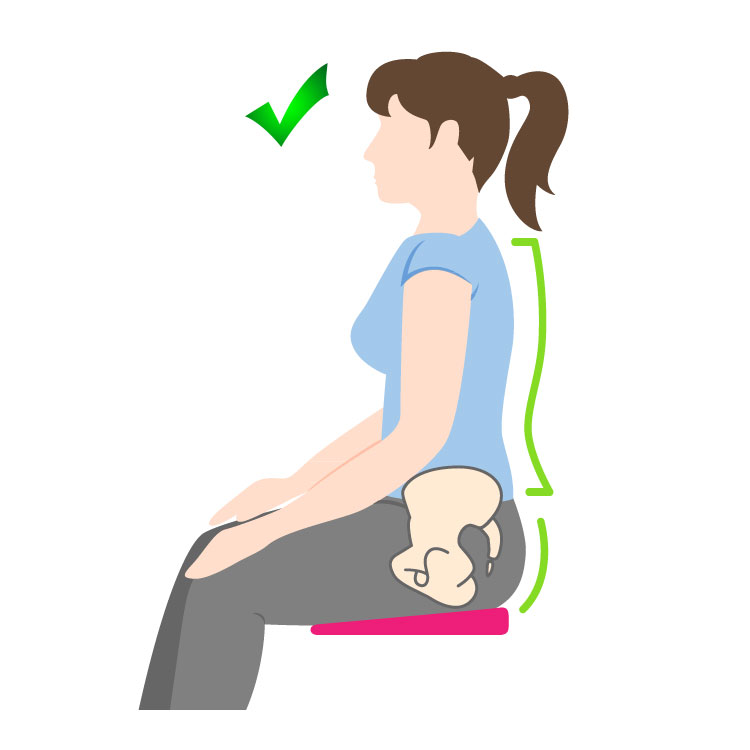
Everything in your body is connected. It’s important to think about this when you’re doing your Kegels, as bad posture causes weak core muscles and a weak pelvic floor. When you slouch, your tailbone tucks underneath you and causes your pelvic floor muscles to contract and stretch which can weaken them.
Hands up if you corrected your posture as you read that…?
As well as weakening them through the day, if you do Kegels in this position you will strain and damage your muscles. Sitting and standing properly ensures that your core and pelvic floor stay toned and active, reducing incontinence and lowering your risk of vaginal prolapse. If you struggle to sit up straight, we recommend a wedge cushion as a way of easing your body into the correct posture while your core gets stronger.
4. Maintain a Healthy Weight
You might know that carrying excess weight around can cause various health problems such as diabetes and high blood pressure. But did you know that it can also cause pelvic floor problems?
The heavier you are, the more likely you are to have a pelvic floor disorder, with 44% of obese and 57% of morbidly obese women suffering from pelvic issues. This is compared to around 33% of women of a healthy weight. The National Institute for Heath and Care Excellence (NICE) recommend keeping your BMI under 30 to avoid causing damage to your pelvic floor.
Being overweight puts lots of extra strain on your pelvic floor muscles, causing stress incontinence (the inability to hold in urine when you cough, laugh, lift, sneeze, run or jump) and prolapses. One study found that 10% weight loss, when combined with pelvic floor exercises, can lead to the pelvic floor muscles becoming up to 50% stronger!
5. Conquer Constipation

If you often find yourself straining to go to the toilet then you're also putting strain on your pelvic floor muscles. This is because your rectal muscles are part of your pelvic floor. In extreme cases this can cause not just a vaginal prolapse, but a rectal prolapse and faecal incontinence.
There are a couple of things you can do to reduce this risk and enable yourself to go more comfortably:
- eat plenty of fibre-packed fruit and vegetables
- drink lots of water
- bring your knees up when on the toilet - using a toilet stool puts your body at just the right angle to empty your bowels easily, protecting your pelvic floor

6. Take Daily Vitamin D3 Supplements
Nutrition is really important for the health of all of your muscles, with Vitamin D being particularly vital. Vitamin D deficiency can cause weakness and a loss of muscle mass, and is associated with a higher risk of incontinence and pelvic floor disorders.
Vaginal prolapse happens when your pelvic floor muscles are weak, so by making sure that you get enough Vitamin D you can decrease your risk of developing this condition. We recommend taking a daily supplement of Vitamin D to protect your pelvic floor and improve the result of your Kegel (pelvic floor) exercises.
7. Choose Your Exercise Carefully
Exercise is one of the most beneficial things you can do for both your physical and mental health. Unfortunately though, if your pelvic floor is weak then there are some forms of exercise that can increase the strain on your muscles.
Any kind of high impact exercise like running, plyometrics (jump training), weight lifting or contact sports creates a lot of force and pressure in your body, potentially weakening your pelvic floor and causing pelvic organ prolapse.
If you don’t want to miss out on the exercise you love, you can reduce the stress that exercise has on your body by wearing good footwear and specialist gear like EVB Sports Support Shorts.
If you know that your pelvic floor is weak or you’ve recently had a baby then it’s best to avoid high impact exercise, at least for now. Good alternatives for maintaining your strength and health include swimming, cycling and yoga.
Follow our advice, and you could prevent yourself ever having to suffer a vaginal (pelvic organ) prolapse. Don't forget to spread the word and share this knowledge with your family and friends. You never know who you might help!
Sources
Choi, K. H Hong, J. Y. (2014) Korean Journal of Urology. Management of Pelvic Organ Prolapse. [online] 55(11), p 693-702. [viewed 20/03/2018]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4231145/
Cochrane, B. Hendrix, S. L. Howard, B. V. Iglesia, C. B. Kudish, B. I. Larson, J. Richter, H. E. Sokol, R. J. (2009). Obstetrics and Gynecology. Effect of Weight Change on Natural History of Pelvic Organ Prolapse. [online] 113(1), p 81-88. [viewed 23/03/2018]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2684063/
Farag, K. A. Uzoma, A. (2009) Obstetrics and Gynecology. International. Vaginal Vault Prolapse. [online] 275621, p1-9. [viewed 21/03/2019]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2778877/
Giarenis, I. Robinson, D. (2014). F1000Prime Reports. Prevention and management of pelvic organ prolapse. [online] 6(77). [viewed 27/03/2018]. Available from: http://f1000researchdata.s3.amazonaws.com/f1000reports/files/9008/6/77/article.pdf
International Urogynecological Association. (2011). Recovery following vaginal repair surgery / vaginal hysterectomy. [online] International Urogynecological Association, 2011
NHS. (2017). What are pelvic floor exercises? [online] National Health Service, 2017. [viewed 23/03/2018]. Available from: https://www.nhs.uk/chq/pages/1063.aspx?categoryid=52
NICE. (2015). Urinary incontinence in women: management, 1 Recommendations [online] National Institute for Health and Care Excellence, 2015 [viewed 14/03/2018]. Available from: https://www.nice.org.uk/guidance/cg171/chapter/1-Recommendations#physical-therapies
Propagator Ltd. (2018). squeezy [online] Propagator Ltd, 2018 [viewed 29/03/2018]. Available from: http://www.squeezyapp.co.uk/
Royal College of Obstetricians and Gynaecologists. (2013). Information for you, Pelvic organ prolapse [online] Royal College of Obstetricians and Gynaecologists, 2013 [viewed 14/03/2018]. Available from: https://www.rcog.org.uk/globalassets/documents/patients/patient-information-leaflets/gynaecology/pi-pelvic-organ-prolapse.pdf
Royal College of Obstetricians and Gynaecologists. (2018). Menopause and women's health in later life, Pelvic organ prolapse [online] Royal College of Obstetricians and Gynaecologists, 2018 [viewed 14/03/2018]. Available from: https://www.rcog.org.uk/en/patients/menopause/pelvic-organ-prolapse/




