I Think I Have A Prolapse?
If you think you have a prolapse you need to be diagnosed
We understand how desperate and frightened you feel, but urge you to take positive steps and not ignore and avoid this difficult situation.
When there's something not quite right with your pelvic floor you know. The first thing you must do however is get a proper diagnosis from your GP. No if's no but's - if you don't know what kind of prolapse (i.e. what organ has fallen downwards, it could be your bladder, cervix, or bowel) or what 'grade' it is (how far it’s come down), how can you take care of yourself and make an informed decision of what to do next?


So what are the symptoms of prolapse?
Here are the common symptoms of prolapse you may or may not recognise. However please be aware that some women have no symptoms at all, and only discover they have a prolapse during a routine check-up or smear test.
You may notice:
- A 'dragging' sensation in the vagina or lower back
- Pelvic and/or abdominal pain
- A lump inside or outside the vagina
- Increased difficulty in emptying your bowel
- Dyspareunia (painful sex) or lack of intimate sensation
- Urinary changes such as a slow stream, incomplete emptying, frequency/urgency or stress incontinence
- The quicker you get an accurate diagnosis the quicker you'll be able to decide how best to manage your prolapse.


What does a prolapse feel like?
Some women have no symptoms of prolapse at all - other women report feeling a 'dragging' or 'pelvic heaviness', they may feel or actually see a bulge, and may be struggling to properly empty their bladder or bowel. Conversely, some women are alerted to prolapse when they start to suffer with bladder weakness and can't control their bladder.
We asked Kegel8 users how their prolapse felt:
- 'I have a feeling of something being there that should not be there'
- 'Painful'
- 'It felt like a golf ball and was very uncomfortable''A constant hanging feeling which is always noticeable, this causes stress and depression as its always there, paranoid it's getting worse all the time'
Going to your GP for a prolapse examination - what to expect
ITV's Dr Chris Steele says - 'don't leave it; don't put it off, the sooner you do something about prolapse the better'. Your GP will need to carry out an internal pelvic examination by feeling in your pelvic area. During the prolapse examination you'll be asked about any other symptoms such as leaking urine when you cough or sneeze. You may be examined standing upright to fully reproduce the extent of the prolapse and provide your GP with an accurate prolapse diagnosis. If your prolapse is causing continence issues with your bladder or bowel your GP may refer you onto a Continence Clinic.
64% of purchases are GP recommended
Kegel8
GP recommended - it's the home use treatment that is taking the UK by storm
You don't need a doctor to tell you when there's something wrong with your pelvic floor – the signs are clear as day – but speaking to a GP or Specialist can really help you decide where to turn for treatment.
In a recent survey, 64% of customers purchased Kegel8 following a recommendation from their GP, Consultant or Healthcare Professional.


Grades of prolapse or stages of prolapse
Usually your GP will be able to 'grade' your prolapse this is a simple way to describe the extent of the prolapse and is used as a general guide as to how much the prolapsed organ has moved downwards out of position. This is not always scientifically accurate - you might find that your prolapse moves downwards as the day goes along or if you have been on your feet all day. If your GP appointment is in the morning your prolapse may not be as evident as it sometimes can be later in the day. The grades of prolapse used by your GP will be given a more accurate diagnosis when you are referred to a Continence Specialist, Physiotherapist or Gynaecologist. Your GP may diagnose one of three levels of prolapse: Mild or slight prolapse, Moderate prolapse or Severe prolapse.
Mild or slight prolapse
Clinical studies have shown that pelvic floor exercise can help. You may be recommended a course of Physiotherapy and hopefully your GP will also mention Kegel8 Pelvic Toners! Do not waste another minute, please start to strengthen your pelvic floor with targeted exercises as soon as possible.
Moderate prolapse
Again, as with mild or slight prolapse Clinical studies have shown that pelvic floor exercise can help. You may be recommended a course of Physiotherapy and hopefully your GP will also mention Kegel8 Pelvic Toners. Do not delay; you need to get your pelvic floor strong with targeted pelvic floor exercises for prolapse.
Severe prolapse
A referral will help you to consider the options you have which may include management of your prolapse. Management of your prolapse is key at this point, and pelvic floor exercise is vitally important, to prevent further deterioration of your existing prolapse and to prevent other organs from prolapsing too.
Stages of prolapse - Pelvic Organ Prolapse Qualification system (POP-Q)
We know you'll be thinking 'how bad is it?'. You'll be concerned and worried but understanding more about your condition will help you make the right choices. If your GP refers you to a Continence Specialist, Physiotherapist or Gynaecologist they may well use the POP-Q system for measuring and more accurately diagnosing your prolapse. As well as a physical examination, including straining, this may also include urinalysis (measuring how much urine is left in your bladder after you've been to the loo). Ultrasound imaging may be performed and in some cases an MRI scan may be performed if the prolapse is severe to help supplement the physical examination.
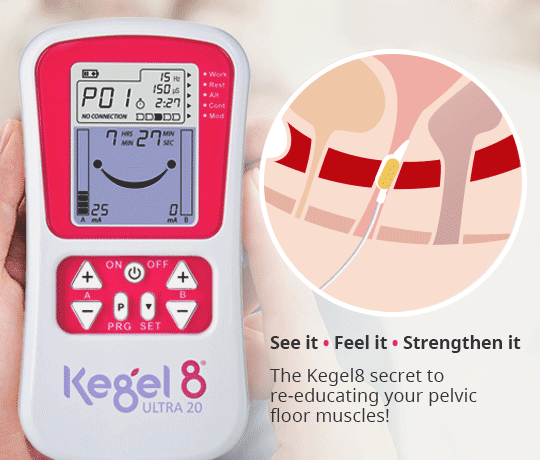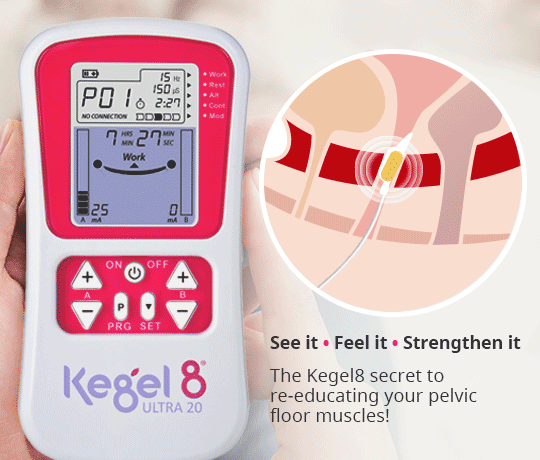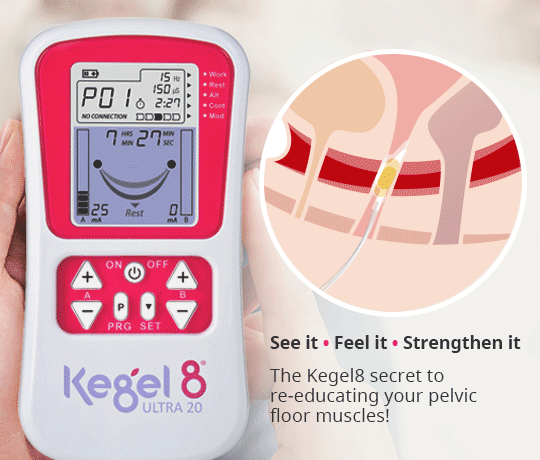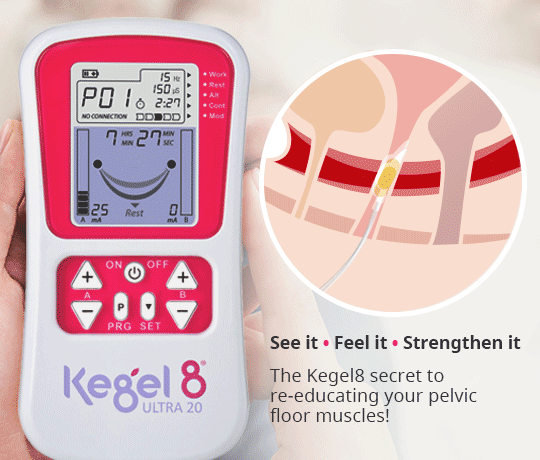
Alleviate the symptoms of pelvic organ prolapse & strengthen the pelvic floor in just 12 weeks, with the help of the Kegel8 Ultra 20 & Amanda Savage!
Amanda Savage is one of the UK’s leading specialist pelvic floor and women’s health physiotherapists, who has worked in the field for over 20 years offering supervised pelvic floor muscle training and support for the recovery of pelvic organ prolapses, incontinence and pelvic surgeries. With post-graduate qualifications, including a master’s degree from the University of Cambridge, she has also gained full membership of the Professional Network of Pelvic, Obstetric & Gynaecological Physiotherapy (POGP). As a Kegel8 ambassador, Amanda Savage has worked alongside us for many years in the development of our best-selling device, the Kegel8 Ultra 20 V2 Electronic Pelvic Toner, to ensure its efficacy. In addition, she has been integral to ensuring all supporting information and instructions are medically accurate so that the device is used correctly/effectively, and treatment is tailored to the specific condition of the user.
Find out more about Amanda Savage, her qualifications, experience, knowledge, and affiliations here.


Comes complete with an easy exercise plan, created by Amanda Savage, to get results in 12 weeks!
Here at Kegel8, we are all too aware of the discomfort, not to mention the anxiety, that is caused by pelvic organ prolapse. So, if you are experiencing an uncomfortable ‘dragging’ sensation, are struggling with bladder and bowel control, bowel emptying and a lack of intimate sensation, you are certainly not alone! Indeed, more common that you may realise, pelvic organ prolapse affects millions of people worldwide. And we are extremely familiar with the impact it has on both physical and emotional well-being, as well as on life in general.
It’s true that, left untreated, the symptoms of pelvic organ prolapse will simply worsen over time. However, they should by no means be accepted as an inevitability! Indeed, regular pelvic floor exercise has been proven to build muscle and tone, creating a thicker support shelf for the organs to rest on. This essentially holds them up and keeps them in place. In addition, much like any other exercise, it builds strength and tone to ensure the muscles do not tire easily and can react quickly to provide additional support during strenuous activities. This improved endurance and strength also helps with bladder and bowel control. So, by simply performing regular pelvic floor exercise, you can get your life back on track!
The included easy exercise plan was created by Amanda Savage to prevent, treat, and alleviate the associated symptoms of pelvic organ prolapse. It is proven to build muscle and tone and create a thicker support shelf for the organs to rest on, essentially holding them up and keeping them in place. In addition, this simple exercise regime will improve endurance and ensure the muscles do not tire as easily, so that they can react quickly and provide the optimum support when performing strenuous activities. This improved endurance and strength also helps with bladder and bowel control and the contractions have been shown to calm the nerves responsible for a sensitive bladder. The plan even encourages the user to practise contracting their muscles alongside the machine, which prepares them for ‘real life’ scenarios when they don’t have access to the machine.
So, why opt for an electronic pelvic floor exerciser rather than performing your Kegels independently?
It is thought that many women push downwards when performing independent pelvic floor exercises, which, rather than strengthening the muscles, can lead to further damage. In addition, it can be difficult to locate and target the correct muscles, making exercise less effective. The Kegel8 Ultra 20 V2 Electronic Pelvic Toner removes the guesswork and essentially acts as a Sat-Nav for your pelvic floor muscles, correctly targeting and stimulating a contraction within them using a small electric current. These contractions build strength and tone in a matter of weeks! With 20 clinically proven pelvic floor exercise programmes which vary in frequency, intensity and duration, the Ultra 20 is proven to treat a variety of different conditions, including pelvic organ prolapse and bladder/bowel control and emptying. And, in addition to tailored programmes, the specific 12-week exercise plans created by Amanda Savage advise exactly how the device should be used, depending upon the condition, to ensure the very best treatment.