Manual vs Electronic Pelvic Floor Toners: Which is Better?
Medically reviewed by Amanda Savage 20/07/2023
If you are struggling to get started with your pelvic floor exercises, or are worried you are not doing them correctly, pelvic exercise tools will improve the efficiency of every squeeze you make. Or, if you’re Kegel-savvy, your pelvic floor exercises will already be second nature and you can use pelvic exercise tools as an added challenge or to mix up your exercise routine.
Manual pelvic floor exercises are defined as those that require you to contract and relax your pelvic floor muscles yourself. You can squeeze against a resistance tool, such as the Kegel8 Kegel Weights (available as an Exercise Set), to work your muscles harder.
Electronic pelvic toners contract and relax your pelvic floor for you, and therefore are not involved in manual exercises. Don’t be mistaken into thinking that electronic toners are a machine for the lazy though; Kegels aren’t easy. In fact, 50% of women don’t know how to perform an effective pelvic floor muscle contraction (and we suspect most of the other 50% simply forget or can’t find the time to do them – correctly or otherwise!) Simply choose one of the pre-set programmes on the device and let the machine do the work.
Completing your pelvic floor exercises with the support of any tool can improve:
- your exercise technique - especially if you struggle to contract the correct muscles.
- the efficiency of your time spent exercising.
- your motivation and as a result you will have a greater likelihood of continuing with a pelvic floor exercise programme.
- your results!
Manual Exercise Tool: Kegel8 Kegel Weights Exercise Set

Many Physiotherapists recommend using resistance / vaginal weights to improve your pelvic floor exercises. They come in varying weights, providing you with progressive exercising. The largest and lightest cone being the easiest to hold in place. Progress to the smallest and heaviest as your pelvic floor strengthens.
The Kegel8 vaginal weights have a unique indicator tail. As you complete your Kegels with the vaginal weights in place, you will see the unique indicator tail demonstrate when you are doing your Kegels well. When you squeeze and lift your muscles correctly, the tail moves down. If the tail moves upwards, you are exercising your bum, thighs or other muscles instead.
If you are in the UK, your GP can prescribe vaginal weights as a treatment for your pelvic floor disorder. Speak to your GP to see if you are eligible.
Manual Exercise Tool: Guides
Using a Physiotherapist approved pelvic floor exercise guide will help keep you motivated and enable you to get the very best out of each squeeze. They are available for both beginners and those that are more advanced.
Electronic Pelvic Toners: Neuromuscular Electrical Stimulation (NMES)
Most electronic pelvic toners use neuromuscular electrical stimulation (NMES) to strengthen your pelvic floor. They work by producing electrical pulses that stimulate the muscles and nerve fibres in your pelvic area. Clinically proven to be more than twice as effective than completing pelvic exercises manually - meaning you can exercise less often and experience even better results.
If you haven’t used a neuromuscular stimulator before, the idea of applying electric pulses to your body can seem a little strange. But there’s no need to be concerned - your body already uses electrical signals all the time. For example, let’s say you want to tense the bicep muscle in your arm. To do this, your brain sends an electrical signal to your muscle via your nervous system. When the signal reaches your bicep, it causes the muscle to contract, and when the signal is not present, your muscle relaxes again. Electronic pelvic toners work in a very similar way - sending electric pulses to precise areas of the weakened muscles in your pelvic area, causing them to contract and relax. Over time, this strengthens the muscles and nerve fibres, giving you greater muscle control and improving tone and tightness. Periods of stimulation are followed by periods of rest, essential in allowing your muscles to heal and not get tight which can otherwise result in pelvic pain.
Some electronic pelvic floor toners, like the Kegel8 Ultra 20 Electronic Pelvic Toner, can be used with skin electrode pads as well as a vaginal probe. Giving your pelvic floor muscles the most effective workout.
Depending on the programme you are using, you will feel your toner complete fast flex and slow flex Kegel exercises. The best way to describe the sensation is a knocking feeling within your pelvis, sometimes accompanied by a tingling. This is how you know you have the current level set correctly for you. Start at a level you are comfortable with, and increase it, as you become used to the sensation, to have a greater effect on your muscles.
To get the most out of your electronic pelvic toner:
- Use an appropriate amount of power - The amount of power needed to stimulate pelvic floor muscles varies from person to person. By default, most electronic pelvic toners start at a 0mAs (milliamps) output. You increase this yourself to a level where you can feel the effects of the electric pulse, but it is not causing any discomfort. Many women find that a setting of around 30mAs is a good starting point with a vaginal probe, but only you can tell what is comfortable for you. If you are using the electrode pads, you should use a lower amount of power - do not exceed 15mA as this could cause you physical harm and may damage your electrodes. As your pelvic floor muscles begin to strengthen, you should find that you can increase the power output.
- Exercise once per day for 12 weeks - We recommend using an electronic toner once a day for 12 weeks. alternate between your choice of programme and a general pelvic floor programme workout each day. When you have better muscle control, you can use a weekly maintenance programme on an ongoing basis to maintain your muscle strength. If you decide to exercise twice a day, it is important that you do not do back-to-back sessions. This is because your pelvic floor muscles need time to recover. We suggest that you use your toner once in the morning and once at night, leaving a gap of at least 8 hours.
- Be patient. Using an electronic pelvic toner WILL improve your pelvic floor - Everybody’s different. Some people respond to electronic pelvic toners very quickly, whereas with others it takes a number of weeks to feel real improvements. But rest assured, if you use the toner regularly, your pelvic floor muscles and nerve fibres will get stronger.
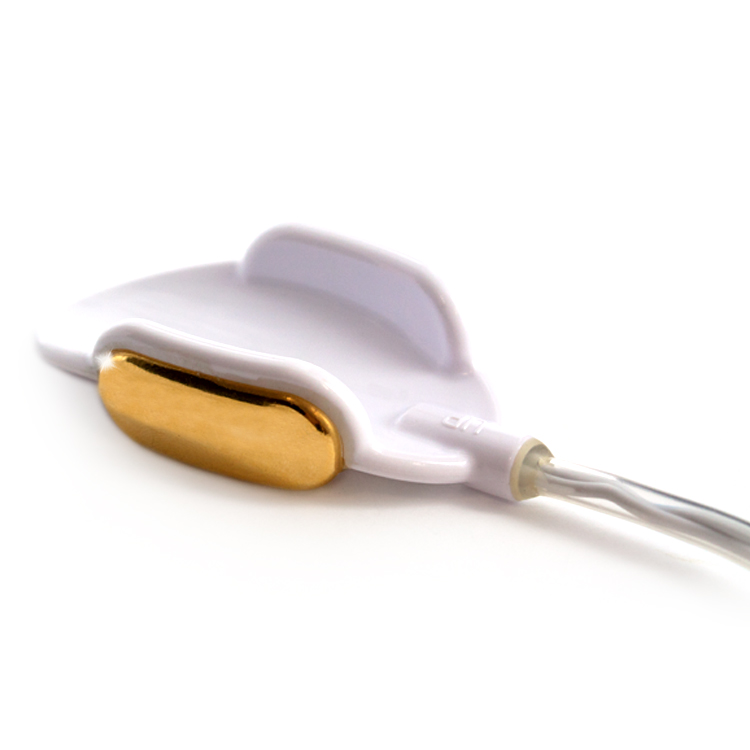
Electronic Pelvic Toners: Vaginal Probes
We understand that using a vaginal probe can be quite daunting, but take comfort in knowing that there are no risks in using one. By using a probe, the mild electrical current is delivered deep into the muscle bed for fast, effective toning and strengthening. You are in control of the level of current that you experience, building it up as you are able. Certain programmes will drop the current when the pulse rate and length is about to increase, just to make sure the change in intensity does not take you by surprise.
Electronic Pelvic Toners: Electrode Pads
If you are concerned or need to be warmed up to the idea to using a vaginal probe, external electrode pads can be used.
The tibial nerve runs down your leg from your pelvis, ending at your ankle. It’s responsible for a lot of your body’s motor functions, including those of your bladder, bowel and pelvic floor. This means that by using tibial nerve stimulation we can ‘wake up’ these areas, returning proper function and curing incontinence. Posterior Tibial Nerve Stimulation (PTNS) uses tiny, painless electrical currents from your electronic toner, passing them up through the skin of your ankle via the electrode pads.
Sacral Nerve Stimulation (SNS) is similar to PTNS, but the nerve begins at your lower back instead of your ankle. The sacral nerves are a group of 31 nerves that reach from your lower back to your rectum, bladder and sphincter and pelvic floor muscles. They help your body to control when your bladder and bowels open and close. Alleviating and, after consistent use, curing both urinary and faecal incontinence, constipation, and urinary retention (the inability to completely empty the bladder).
Take care when increasing the power to your electrode pads as your skin is sensitive. We recommend that you do not increase the power above 15mA, as a power higher than this could cause physical harm (skin burns). Power greater than 15mA could also cause damage to your electrode pads. You should be extra careful when using the probe and electrode pads at the same time, as the probe will need a much higher amount of power (usually 30mA or more).
Sources
Bø, K. Talseth, T. Holme, I. (1999). The BMJ. Single blind, randomized controlled trial of pelvic floor exercises, electrical stimulation, vaginal cones and no treatment in management of genuine stress incontinence in women. [online] 318(7182), p487–93. [viewed 19/12/2024]. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC27740/
Castro, R. A. Arruda, R. M. Zanetti, M. R. D. Santos, P. D. Sartori, P. G. F. Girão, M. J. B. C. (2008). Clinics. Single-Blind, Randomized, Controlled Trial of Pelvic Floor Muscle Training, Electrical Stimulation, Vaginal Cones, and No Active Treatment in the Management of Stress Urinary Incontinence. [online] 63(4), p465-472. [viewed 19/12/2024]. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2664121/
Lang, J. Pang, H. Shi, H. Shi, X. Sun, Z. Wang, W. Zhu, L. (2015). Zhonghua fu chan ke za zhi. Continuous improvement of portable domestic pelvic floor neuromuscular electrical stimulation on the pelvic floor function of patients with urinary incontinence. [online] 50(12), p 937-941. [viewed 19/12/2024]. Available from: https://pubmed.ncbi.nlm.nih.gov/26887879/
Herbison, G. P. Arnold, E. P. (2009). Cochrane Database of Systematic Reviews. Sacral neuromodulation with implanted devices for urinary storage and voiding dysfunction in adults. [online] 15(2). [viewed 19/12/2024]. Available from: https://pubmed.ncbi.nlm.nih.gov/19370596/
NHS Business Services Authority. (2018). NHS Prescription Services, Drug Tariff Part IX. [online] NHS Business Services Authority, 2018. [viewed 19/12/2024]. Available from: https://www.nhsbsa.nhs.uk/pharmacies-gp-practices-and-appliance-contractors/drug-tariff/drug-tariff-part-ix
NHS Trust. (Reviewed 2023). Urinary incontinence, Non-surgical treatment. [online] NHS Trust, 2016. [viewed 19/12/2024]. Available from: https://www.nhs.uk/conditions/urinary-incontinence/treatment/
NICE. (Updated 2023). Urinary incontinence in neurological disease: assessment and management. [online] National Institute for Health and Care Excellence, 2023. [viewed 19/12/2024]. Available from: https://www.nice.org.uk/guidance/cg148/resources/urinary-incontinence-in-neurological-disease-assessment-and-management-pdf-35109577553605
NICE. (Updated 2021). Urinary incontinence in women. [online] National Institute for Health and Care Excellence, 2021. [viewed 19/12/2024]. Available from: https://www.nice.org.uk/guidance/qs77/resources/urinary-incontinence-in-women-pdf-2098853147077
Payne, J. (2017). Lower Urinary Tract Symptoms in Women (LUTS), Pelvic Floor Exercises. [online] Patient, 2017. [viewed 19/12/2024] Available from: https://patient.info/news-and-features/pelvic-floor-exercises
Peattie, A. B. Plevnik, S. Stanton, S. L. (1988).BJOG: An International Journal of Obstetrics & Gynaecology.Vaginal cones: a conservative method of treating genuine stress incontinence. [online] 95(10), p1049–1053. [viewed 19/12/2024]. Available from: https://pubmed.ncbi.nlm.nih.gov/3191043/
Price, N. Dawood, R. Jackson, S. R. (2010). Maturitas. Pelvic floor exercise for urinary incontinence: A systematic literature review. [online] 67(4), p309-315. [viewed 19/12/2024]. Available from: https://www.semanticscholar.org/paper/elvic-floor-exercise-for-urinary-incontinence-%3A-A-Price-Dawood/189c3b354e250e621df819c4dc96ddece0f835ac?p2df





