
With Bonfire Night just around the corner, we can expect to hear a couple of BANG’s and a fair few POP’s. But one POP that you certainly won’t want to hear is Pelvic Organ Prolapse.
What is a Pelvic Organ Prolapse?
Pelvic Organ Prolapse (POP) is a condition where one or more of the pelvic organs (e.g. uterus, bladder, vagina, or rectum) droop from their usual healthy position in your pelvis and fall down.
1 in 12 women living in the UK report symptoms of a pelvic organ prolapse, and 1 in 2 women over the age of 50 are affected by vaginal prolapse.
What Causes a Pelvic Organ Prolapse?
Pelvic organ prolapse can occur when your pelvic floor becomes weakened and can no longer hold the organs in place. Your pelvic floor is a group of muscles and tissues that normally support the pelvic organs, e.g. bladder, bowel.
There are a variety of things that can cause damage to your pelvic floor, these include:
- Pregnancy and childbirth
- The menopause
- Being overweight or obese
- Having a hysterectomy
- Suffering from chronic constipation
- Heavy lifting
Types of Prolapse
Anterior prolapse (Cystocele) – The bladder bulges into the front wall of the vagina
Vault prolapse – The top of the vagina sagging down
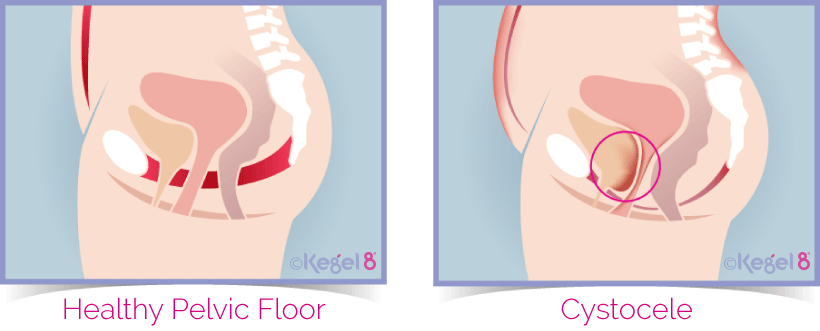

Uterine prolapse – The womb bulges or hangs down into the vagina
Posterior wall prolapse (Rectocele) – The bowel bulges forward into the back wall of the vagina
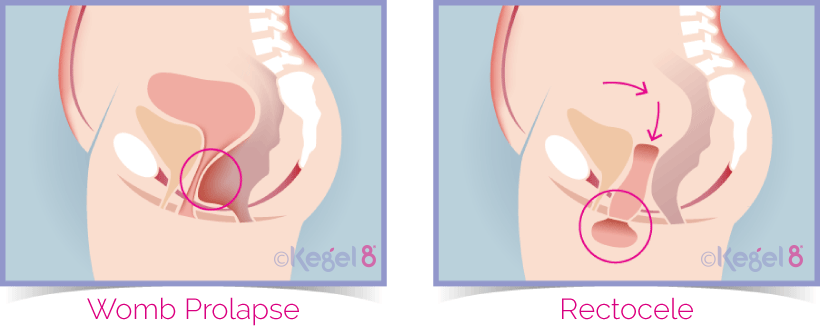

You can suffer from more than one type of prolapse at a time. The prolapse will be classified on a scale from 1 to 4 depending on its severity, with 4 being the most severe.
What are the Symptoms of a Pelvic Organ Prolapse?
Some of the symptoms that you may experience during prolapse are:
- A feeling of heaviness in your pelvis
- A dragging discomfort in your vagina
- Feeling or seeing a bulge or lump in or coming out of your vagina
- A feeling like there is something protruding down into your vagina – it may even feel like you are sitting on a small ball
- Numbness or discomfort during sex
- Problems with urinating, e.g. experiencing stress incontinence or an overactive bladder
In some cases, a POP has no symptoms at all and can be found during an internal examination, e.g. in a cervical screening.
How to Prevent and Treat a Pelvic Organ Prolapse
If your prolapse is mild, a few simple lifestyle changes can ease your symptoms and prevent the prolapse from worsening. They can also reduce the risk of developing POP in the first place. These include:
- Doing regular pelvic floor exercises to keep the muscles strong and supportive
- Maintaining a healthy weight
- Avoiding constipation by eating a high-fibre diet
- Avoid heavy lifting
- Avoiding high-impact exercise
- Quitting smoking – coughing can make the prolapse worse
If non-surgical options do not work, or the prolapse is severe, surgery may be considered. Surgical treatments include:
- Surgical repair – Surgery that lifts and supports the pelvic organs by stitching them into place or supporting existing tissues.
- Hysterectomy – Surgery to remove the womb can help relieve pressure on the vaginal walls.
- Colpocleisis – Closing all or part of the vagina. This is only offered to women with severe prolapse who don’t plan on having sexual intercourse again in the future.
Kegel8’s Top Tips for Supporting Your Pelvic Floor This Bonfire Night
- Remember remember to Kegel in November – It’s vital that you perform your pelvic floor exercises to strengthen the muscles and provide support to the organs. Try performing a pelvic floor contraction each time a firework booms.
- Remember remember to never surrender – In some cases, you may not see any improvement for at least 12 weeks of exercising. It’s important that you don’t give up! To check that you are doing your Kegels correctly, try using a biofeedback device, or try the Kegel8 Ultra 20 to contract the correct muscles for you.
- Remember remember it’s not based on gender – Both males and females can suffer from a pelvic organ prolapse, so no one has an excuse not to Kegel.
Sources
[1] Cooper, J., et al. (2015) Prevalence of genital prolapse symptoms in primary care: a cross-sectional survey. International Urogynecology Journal. 26(4), pp. 505-510.
[2] NHS (2018) Pelvic Organ Prolapse [online]. NHS [viewed 30/10/2018]. Available from https://www.nhs.uk/conditions/pelvic-organ-prolapse/
[3] NHS (2018) Pelvic Organ Prolapse Treatment [online]. NHS [viewed 30/10/2018]. Available from https://www.nhs.uk/conditions/pelvic-organ-prolapse/treatment/
[4] Onwude, J.L. (2009) Genital Prolapse in Women. BMJ Clinical Evidence. Available from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2907774/




