Pigs in blankets. Stuffing balls. Even brussel sprouts. Just name it, and you can guarantee that you’ve eaten it over Christmas. But whilst you’re lying there, basking in your food coma, something takes you by surprise. PRRP! Was that you? Oh no, time to rush to the toilet!
We often see this as a comedic event, but in reality, 1 in 10 people are affected by bowel incontinence at some point in their lives – this can be a one-off or an everyday occurrence. Sound familiar? Read on to learn more.
What is Bowel Incontinence?
Bowel incontinence concerns the involuntary leakage of stool and/or gas.
Your bowel is responsible for absorbing nutrients and fluid from the food and drink that you consume, before the waste is removed from your body.
What Causes Bowel Incontinence?
The nerve endings in the rectum are stimulated by waste, resulting in the urge for bowel movement. This in turn stimulates your internal muscles to involuntarily relax and open.
Usually, we consciously keep this muscle tight and closed, until we are on the toilet, where we can relax it and allow defecation to occur. But, issues can start to arise if you have weak or damaged pelvic floor muscles.
Bowel incontinence is recognised as three separate types of incontinence:
- Faecal bowel incontinence – The inability to control leakage of faeces and gas.
- Flatus bowel incontinence – The inability to control the leakage of gas.
- Double incontinence – The involuntary leakage of urine, faeces and gas.
The main causes of incontinence include:
- Pregnancy and Childbirth – Due to the damage that occurs to the pelvic floor during pregnancy and labour, many women suffer with incontinence as a result. In fact, faecal incontinence affects 25% of women!
- Age – As we grow older, our pelvic floor muscles become naturally weaker. This means that we are more susceptible to developing a pelvic floor disorder. Read on to learn how to prevent this.
- Obesity – Excess weight can cause a huge strain on your pelvic floor muscles. Not only can this lead to incontinence, but it can make any pre-existing incontinence even worse!
- High Impact Exercise – Exercises such as running, and weight lifting can really take a toll on your pelvic floor. Click here to learn about other exercises that damage your pelvic floor.
- Pelvic Organ Prolapse – 60% of women with a prolapse also suffer from urinary incontinence.
How to Prevent Bowel Incontinence?
Kegel8’s top tips on preventing bowel incontinence includes:
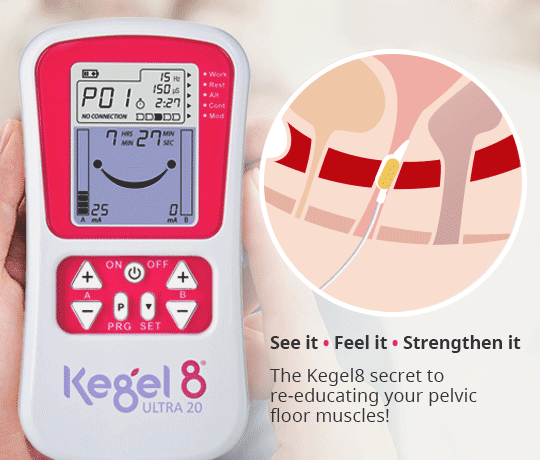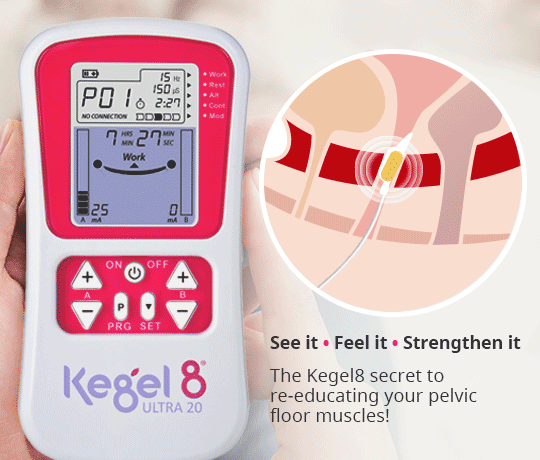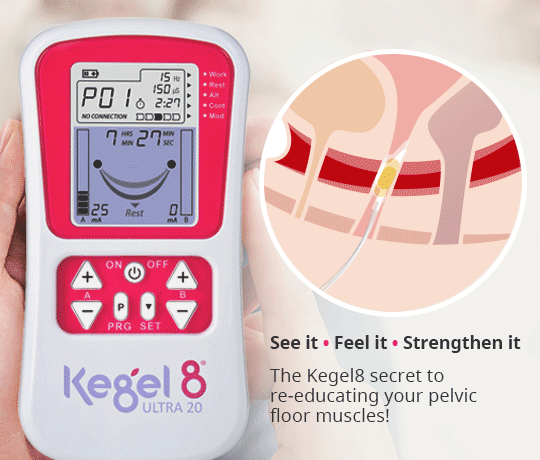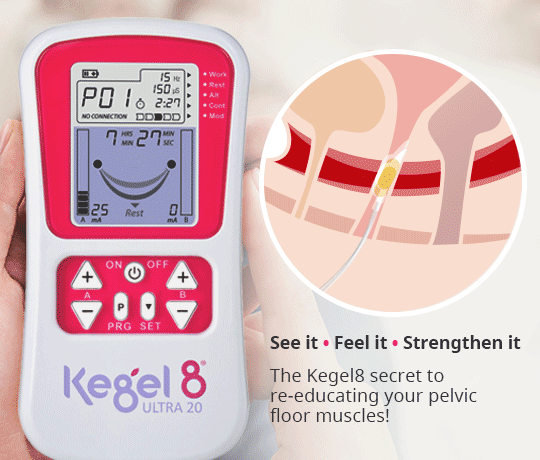
- Kegel! – Strong pelvic floor muscles are vital in your ability to control your bladder and bowel. Pelvic floor exercises can reduce the frequency of incontinence episodes by half within 6 weeks! If you find it difficult to contract the correct muscles, you may not see an improvement in your incontinence. In this case, you can use an electronic pelvic toner to quicken improvements. The Kegel8 Ultra 20 Electronic Pelvic Toner has specialised, medically approved programmes that can help to resolve your specific form of incontinence. Learn more about the Ultra 20 here!
- Stop straining – Constipation can put added strain on your pelvic floor. To avoid this, ensure your fibre intake is healthy and use a toilet stool to optimise your toilet sitting position.
- Maintaining a healthy weight – Reducing your weight by just 5% can cut your incontinence episodes in half!
- Stop smoking – The chronic cough that you develop alongside smoking can weaken your pelvic floor.
Incontinence Treatment – Surgery
If conservative treatments or medicines are not effective enough for you, you may choose to opt for surgical treatment. In this case, a few of your options include:
- Uterine fibroids removal (women) – Popular procedures for this removal include: Myomectomy (removal of fibroids from uterus), Hysterectomy (removal of the womb), and Non-surgical uterine fibroid embolization (deprive fibroid of blood supply).
- Bladder enlargement – The size of your bladder is increased by adding a piece of intestinal tissue.
- Sacral nerve stimulation – A device can be fitted at the bottom of your back that stimulates your muscles. This can help to reduce incontinence episodes and constipation.
Whether you suffer from incontinence or want to preserve your bowel health, start Kegeling today and together we will be stronger!
Reviews for the Kegel8 Ultra 20 Electronic Pelvic Toner
Becky - At Last - A Product That Works!
"Having had two repairs each for prolapsed bladder and bowel just over a year ago, I was devastated to find I had another small bladder prolapse. Surgeon has suggested further surgery. I had previously purchased a similar product to Kegel8 some years ago and felt it didn't make any difference, although I did use regularly. Took the plunge and bought the Ultra 20 a couple of weeks ago. Within days of using I can feel the difference. No longer do I have vaginal noise and a feeling of fullness and dragging. Better still I no longer have to use pads "just in case". I have been referred to a continence nurse in preparation for surgery to ensure that I know how to do my pelvic floor exercises. I have deferred the appointment, because I have confidence that if used regularly the Ultra 20 will work. My husband has already commented that there is a marked difference - if it can do that in two weeks then I am looking forward to the three month results!! ”
Jude - Fantastic, Best Choice I Made!
"I bought this as I have a bit of prolapse and no pelvic floor strength. I saw a physio who, after examining me, said I needed to purchase the Ultra 20 as exercises alone were not enough. Since purchasing this I haven't looked back. My pelvic floor is improving and so is everything else, including in the bedroom! My only regret is that I didn't buy it sooner. I have been using it twice a day for four weeks. The difference is unbelievable. Things will just keep getting better. I phoned the helpline for advice and they were amazing. I cannot rate this highly enough. It's brilliant!”
Sources
[1] Altman, D. Falconer, C. Rossner, S. Melin, I. (2007). International Urogynecology Journal. The risk of anal incontinence in obese women. [online] 18(11), p1283-1289 [viewed 26/04/18]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/17356799
[2] Bladder and Bowel Support Company (2018b). Faecal Incontinence. [online] Bladder and Bowel Community. [viewed 25/04/18]. Available from: https://www.bladderandbowel.org/bowel/bowel-problems/faecal-incontinence/
[3] Buchsbaum, G. M. (2006). Minerva Urologica e Nefrologica. Urinary incontinence and pelvic organ prolapse. [online] 58(4), p311-319. [viewed 27/04/18]. Available from: https://www.ncbi.nlm.nih.gov/pubmed/17268396
[4] Dwyer, N. T. (2006). Urology Board Review Manual. Stress Urinary Incontinence in Women. [online] 13(1), p 1-12.
[5] Hull, T. (2007). Clinics in Colon and Rectal Surgery. Fecal Incontinence. [online] 20(2), 118-124. [viewed 26/04/18]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2780180/
[6] Melville, J. L. Fan, M. Y. Newton, K. Fenner, D. (2005) American Journal of Obstetrics & Gynecology. Fecal incontinence in US women: A population-based study. [online] 193(6), p2071-2076. [viewed 26/04/18]. Available from: https://www.ajog.org/article/S0002-9378(05)01087-2/fulltext
[7] National Institute of Diabetes and Digestive and Kidney Diseases. (2015). Bladder Control Problems in Men (Urinary Incontinence)[online] National Institute of Diabetes and Digestive and Kidney Diseases, 2015. [viewed 23/04/18]. Available from: https://www.niddk.nih.gov/health-information/urologic-diseases/bladder-control-problems-men
[8] NHS Inform (2018) Bowel incontinence [online]. NHS 24 [viewed 10/12/2018]. Available from https://www.nhsinform.scot/illnesses-and-conditions/stomach-liver-and-gastrointestinal-tract/bowel-incontinence
[9] NICE, (2013). Urinary incontinence in women: management. National Institute for Health and Care Excellence, 2015. [viewed 18/04/18] Available from: https://www.nice.org.uk/guidance/cg171/resources/urinary-incontinence-in-women-management-pdf-35109747194821
[10] Price, N. Dawood, R. Jackson, S. R. (2010). Maturitas. Pelvic floor exercise for urinary incontinence: A systematic literature review. [online] 67(4), p309-315. [viewed 16/04/18]. Available from: https://pdfs.semanticscholar.org/bd40/19fc898987cfb343c6652205837f92029039.pdf
[11] Royal College of Nursing. (2016). Causes of incontinence. [online] Royal College of Nursing, 2016. [viewed 23/04/18]. Available from: https://rcni.com/hosted-content/rcn/continence/causes-of-incontinence
[12] Varma, M.G., et al. (2006) Fecal Incontinence in Females Older Than Aged 40 Years: Who is at Risk? Dis Colon Rectum. 49(6): 841-851.