It’s pretty common knowledge now that you should be exercising your pelvic floor. If you haven’t heard of Kegels where have you been?! For those out of the loop – Kegels are a form of exercise that specifically target your pelvic floor muscles; often a set of voluntary contractions to strengthen the muscles.
When you perform a Kegel exercise you should ALWAYS remember to relax your pelvic floor after contracting it. Failing to teach your pelvic floor muscles how to relax can lead to them becoming overactive – this can be seen in certain activities, such as ballet, where the pelvic floor plays a big role.
Why is the pelvic floor important in ballet?
In ballet, dancers rely heavily on their abdominals, back, and pelvic muscles in order to maintain the correct stance, stay stable, and balance their weight. The pelvis ultimately helps to support torso movement and coordinate the action of a ballerina’s limbs.
You may think of the core as just your abdominals – but it’s best to think of it as a cylinder. Your back muscles and diaphragm are at the top, and your pelvic floor supports it all from the bottom. These two components play a huge part in stability during ballet and help to reduce strain on the abs and back muscles.
What pelvic floor problems are associated with ballet?
Repetitive movement can overload the pelvic floor muscles. This can be caused by tasks that require repetitive movement in the same way for long periods of time, such as ballet.
Ballet dancers also often demonstrate a tendency to stand with a flattened back and use an altered breathing pattern. This, combined with pulling down on their lower abs and ribcage to maintain their posture, can stress the pelvic floor muscles. This can result in pelvic pain or can increase the risk of developing a pelvic floor disorder.
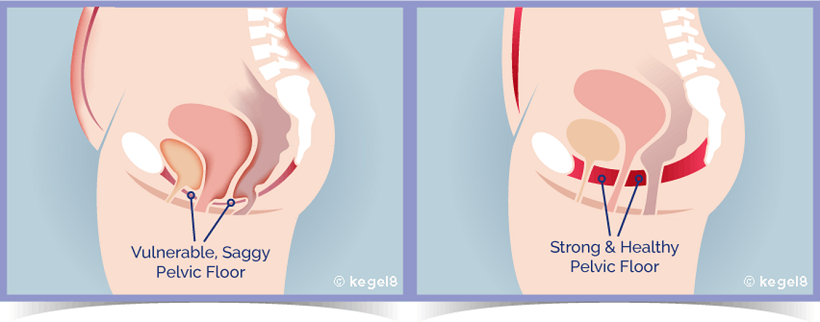
When the pelvic floor muscles constantly contract (often without realising), your pelvic floor may become overactive. Problems that can develop from an overactive pelvic floor include:
- Incontinence – A slow urine flow, accidental leakage, inability to completely empty the bladder and urinary urgency can all result from a lack of pelvic floor muscle relaxation. 43% of ballet dancers experience urinary leakage, with jumping being the largest contributing activity. Dancers can also experience incontinence during their daily life. A 2007 study found that stress urinary incontinence was triggered by dance in nearly 70% of females with urinary incontinence.
- Bowel problems – Incomplete emptying of stool, constipation, and difficulty in commencing bowel movement can result from overactive pelvic floor muscles. Straining to go can also lead to increase pelvic floor muscle pain and tension; this can cause further issues such as a rectal prolapse, haemorrhoids or anal fissures. To combat straining, try using a toilet stool to reduce straining by 90%!
- Decreased intimate sensation – Suffering from overactive pelvic floor muscles can lead to issues with intercourse and penetration. Vaginismus is a condition that can occur where the pelvic floor muscles spasm involuntarily during vaginal penetration. This can prevent intercourse, tampon use, and gynaecological exams.
- Pelvic pain – Pelvic floor muscle tension can produce a pain, ache or discomfort in the lower abs, back or in and around the vagina or anus.
- Pelvic floor muscle weakness – If the pelvic floor muscles are contracted too much they can tire out and become significantly weak. If weakened, they may not work as required, leading to issues such as stress incontinence.
- Difficulty in childbirth – Tight pelvic floor muscles are thought to impair the progress of labour and can result in instrumental deliveries.

What is the treatment for a weak pelvic floor?
The leading treatment for overactive pelvic floor muscles is pelvic floor rehabilitation therapy.
Biofeedback is an effective neuromuscular training approach where patients can learn how to correctly contract, and more importantly, relax their muscles. Clinical trials have demonstrated that biofeedback therapy to improve anal and pelvic floor relaxation improves symptoms in defecatory disorders.
Sources
[1] Fall M, Baranowski AP, Elneil S, et al. (2010) EAU guidelines on chronic pelvic pain. European Urology. 57(1), pp. 35-48.
[2] Faubion, SS., Shuster, LT., Bharucha, AE. (2012) Recognition and Management of Nonrelaxing Pelvic Floor Dysfunction. Mayo Clinic Proceedings. 87(2), pp. 187-193.
[3] Faubion, SS., Shuster, LT., Bharucha, AE. (2012) Recognition and Management of Nonrelaxing Pelvic Floor Dysfunction. Mayo Clinic Proceedings. 87(2), pp. 187-193.
[4] Howard, F. Pelvic Pain: Diagnosis and Management. Philadelphia: Lippincott Williams & Wilkins, 2000.
[5] Howse, J., McCormack, M. Anatomy, Dance Technique and Injury Prevention. (London: A & C Publishers Ltd, 2009), p. 56.
[6] Keynes R, Aidley D, Huang C. Nerve and Muscle. Cambridge: Cambridge University Press, 2011.
[7] Philips, C. (2005). Stability in dance training. Journal of Dance Medicine and Science, 9(1), 24-28.
[8] Pozo-Municio, C. (2007) Genitourinary Conditions in Young Dancers Relationship Between Urinary Incontinence and Foot Flexibility. Journal of Dance Medicine and Science. 11(2).
[9] Thyssen, HH., Clevin, L., Olesen, S., Lose, G. (2002) Urinary incontinence in elite female athletes and dancers. International Urogynecology Journal. 13(1), pp. 15-17.
[10] Tu F.F., As-Sanie S., Steege J.F. (2005) Musculoskeletal causes of chronic pelvic pain: a systematic review of existing therapies: part II. Obstetrical and Gynecological Survey. 60(7), pp. 474–483.
[11] Whitehead W.E., Bharucha A.E. (2010) Diagnosis and treatment of pelvic floor disorders: what's new and what to do. Gastroenterology. 138(4), pp. 1231–1235.