Help & Advice
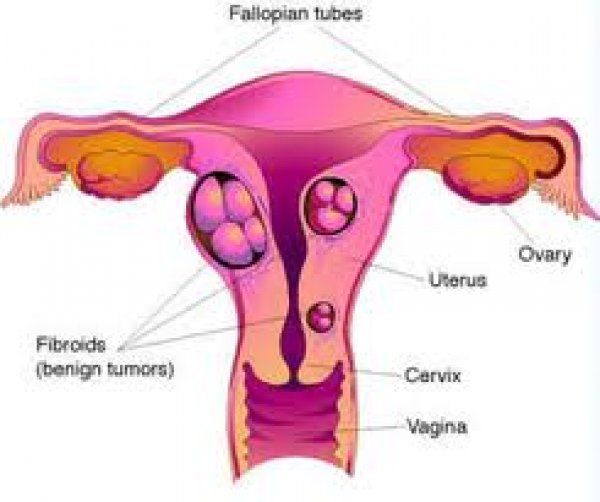 Fibroids, or uterine fibroids, are small growths that grow in and around the womb. They are non-cancerous and most of the time, women don’t even know that they have them. Fibroids are often discovered by chance during routine pelvic examinations or scans. However they can also cause problems such as pain or heavy bleeding.
Fibroids, or uterine fibroids, are small growths that grow in and around the womb. They are non-cancerous and most of the time, women don’t even know that they have them. Fibroids are often discovered by chance during routine pelvic examinations or scans. However they can also cause problems such as pain or heavy bleeding.
If fibroids cause problems, they can be treated with medication, however if this is not successful, surgery may be recommended.
Types of Fibroids
Intramural fibroids - grow in the uterine wall and are the most common type of fibroid.
Submucosal fibroids - grow on the inside of the womb (uterus) and extend into the uterine cavity.
Subserol fibroids - grow on the lining between the uterus and the pelvic cavity (outisde of the womb).
The Kegel8 Guide to Fibroid Surgery
There are a number of different surgical alternatives available for the treatment of fibroids if they become a problem. The type of surgery that...
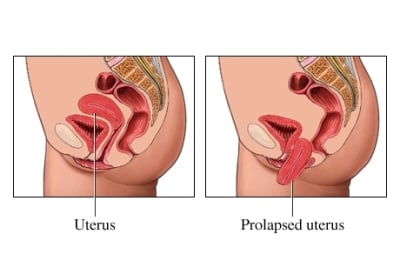
Pelvic organ prolapse occurs when one of your pelvic organs ‘drops’ because it is no longer held in the correct position. There are four stages of prolapse, 1 being the mildest and 4 being the most severe – stage 3 and 4 are also known as procidentia, which means the prolapsed organ protrudes out of the body.
Any pelvic organ can prolapse, and common prolapse conditions include bladder prolapse (cystocele), urethral prolapse, uterine (womb) prolapse, vaginal vault prolapse, bowel prolapse (enterocele) and rectal prolapse (rectocele).
Before resorting to surgery, there are other, more conservative treatment options for prolapse, including pelvic floor exercise (which we of course recommend strongly) and the use of a vaginal pessary. However, if your surgeon decides...
Undergoing a hysterectomy is a life changing experience. 1 in 5 UK women will have a hysterectomy by the age of 60 yet it seems to be one of those taboos that are never discussed! This leads to many women not having the information they need to make the right lifestyle choices. Here at Kegel8 we believe that women’s health issues aren’t something that should be swept under the rug. Given our specialism in the workings of the pelvic floor, we wanted to create a guide especially for those of you who’ve had hysterectomies. We hope that this information will empower you to feel in control of your body post-surgery and live a full and happy life!

Recovering from Your Operation – The First 6 Weeks
As...
You might have heard of your pelvic floor muscles, also known as your Kegel or PC muscles. These all refer to the same collection of muscles, fibres and ligaments that work together to support your pelvic organs and give you urogenital control (control of both urinary and genital organs) in your pelvic floor.
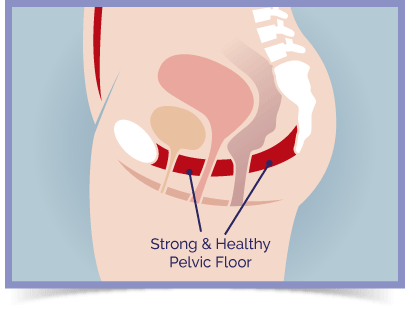
The pelvic floor is made up of three main layers of muscle:
- The superficial group - This is the group of muscles that are found at the entrance to the vagina in women. They help with sexual function and help you to control the bladder. These muscles can weaken as a result of childbirth, the menopause, or gradually as you age.
- The urogenital muscle group - This is the group of muscles that surround the urinary and...
The group of muscles that make up the pelvic floor work in the same way as any other muscle in the body. Relaxing and contracting to move the surrounding ligaments, bones and organs. The only voluntary function of the pelvic floor muscle is the same contraction you do for your pelvic floor exercises; an inward lift and squeeze around your vagina, rectum and urethra.
But what do the pelvic floor muscles do when they contract and relax?
- Healthy urination and bowel movements - A strong pelvic floor is essential to have voluntary movement of both the sphincter and urethra. They must coordinate to have a full bowel movement. Hence the weakening of these muscles often results in incontinence or conversely, constipation.
- Aids sexual function - Alongside a variety of psychological and biological issues, the pelvic floor muscles are essential in satisfactory erectile function and ejaculation...
Kegel exercises work your pelvic floor muscles and can help with both urinary incontinence and sexual dysfunction. It's extremely unlikely that you'll injure yourself doing these exercises, but you can still overdo them to the point of mild to moderate pain. The biggest risk of overdoing Kegels is temporary muscle pain, often in the vagina or around the rectum. It's extremely unlikely that you'll tear or otherwise injure your PC muscles, but if you experience pain, burning or stretching, take a break from Kegels until the pain goes away. If the pain gets worse or is severe, avoid Kegels and call your doctor for advice. Follow our handy guide to help you exercise safely and get the best results...
Our years of experience in helping people to cure and prevent pelvic floor disorders have given us a lot of insight into the best way to protect these delicate muscles. By paying a little bit of extra attention to these 6 parts of your life you can futureproof your pelvic floor muscles and ensure you stay healthy and happy!
1. Pelvic Floor Exercises
We’re passionate about the need for everyone to keep up with their kegel exercises, and the facts back us up! Pelvic floor exercises are recommended by medical professionals around the world as the best way to tackle pelvic disorders. Symptoms like incontinence and prolapse are massively reduced and even totally cured, in just a few minutes a day!
What is My Pelvic Floor?
- More Effective Pelvic Floor Exercises Condition Guide
- Bladder Weakness & Stress Incontinence Condition Guide
- Uncontrollable Gas/Wind & Lack of Bowel Control Condition Guide
- Perimenopause, Menopause & Post Menopause Condition Guide
- Pelvic Organ Prolapse Condition Guide
- Postpartum Recovery Condition Guide
- Vaginal...
- More Effective Pelvic Floor Exercises Condition Guide
- Bladder Weakness & Stress Incontinence Condition Guide
- Uncontrollable Gas/Wind & Lack of Bowel Control Condition Guide
- Perimenopause, Menopause & Post Menopause Condition Guide
- Pelvic Organ Prolapse Condition Guide
- Postpartum Recovery Condition Guide
- Vaginal...
- More Effective Pelvic Floor Exercises Condition Guide
- Bladder Weakness & Stress Incontinence Condition Guide
- Uncontrollable Gas/Wind & Lack of Bowel Control Condition Guide
- Perimenopause, Menopause & Post Menopause Condition Guide
- Pelvic Organ Prolapse Condition Guide
- Postpartum Recovery Condition Guide
- Vaginal...
- More Effective Pelvic Floor Exercises Condition Guide
- Bladder Weakness & Stress Incontinence Condition Guide
- Uncontrollable Gas/Wind & Lack of Bowel Control Condition Guide
- Perimenopause, Menopause & Post Menopause Condition Guide
- Pelvic Organ Prolapse Condition Guide
- Postpartum Recovery Condition Guide
- Vaginal...
- More Effective Pelvic Floor Exercises Condition Guide
- Bladder Weakness & Stress Incontinence Condition Guide
- Uncontrollable Gas/Wind & Lack of Bowel Control Condition Guide
- Perimenopause, Menopause & Post Menopause Condition Guide
- Pelvic Organ Prolapse Condition Guide
- Postpartum Recovery Condition Guide
- Vaginal...



